Mpox clade I outbreak
An outbreak of mpox clade I is ongoing. Monitor the news and outbreak sections on this page for updates.
General Information
The information on these pages should be used to research health risks and to inform the pre-travel consultation.
Travellers should check the Foreign, Commonwealth & Development Office (FCDO) country-specific travel advice page (where available) which provides information on travel entry requirements in addition to safety and security advice.
Travellers should ideally arrange an appointment with their health professional at least four to six weeks before travel. However, even if time is short, an appointment is still worthwhile. This appointment provides an opportunity to assess health risks taking into account a number of factors including destination, medical history, and planned activities. For those with pre-existing health problems, an earlier appointment is recommended.
All travellers should ensure they have adequate travel health insurance.
A list of useful resources including advice on how to reduce the risk of certain health problems is available below
Resources
Mpox clade I outbreak
An outbreak of mpox clade I is ongoing. Monitor the news and outbreak sections on this page for updates.
Vaccine Recommendations
Details of vaccination recommendations and requirements are provided below.
All travellers
Travellers should be up to date with routine vaccination courses and boosters as recommended in the UK according to their age, medical history and individual risks.
Current routine UK vaccination schedule
The travel health consultation provides an opportunity to check whether routine immunisations are up to date such as MMR/MMRV and diphtheria-tetanus-polio vaccines. The following link provides information on the current recommended immunisation schedule recommended in the UK.
Country-specific diphtheria recommendations are not provided here. Diphtheria, tetanus and polio are combined in a single vaccine in the UK. Therefore, when a tetanus booster is recommended for travellers, diphtheria vaccine is also given. In the event of a diphtheria outbreak in a country, specific diphtheria vaccination guidance will be provided.
Vaccination of individuals with uncertain or incomplete immunisation
For individuals with an uncertain or incomplete immunisation history please find guidance for health professionals here Vaccination of individuals with uncertain or incomplete immunisation.
UKHSA provide an immunisation comparison tool for individuals who may have been vaccinated overseas UK and international immunisation schedules comparison tool.
Selective immunisation programmes
Those who may be at increased risk of an infectious disease due to their work, lifestyle choice, or certain underlying health problems should be up to date with additional recommended vaccines. See vaccine recommendations for these groups at the bottom of the 'Complete routine immunisation schedule' document. The individual disease chapters of the 'Green Book' Immunisation against infectious disease provides further details.
Certificate requirements
Please read the information below carefully, as certificate requirements may be relevant to certain travellers only. For travellers further details, if required, should be sought from their healthcare professional.
- There is a risk of yellow fever transmission in parts of Kenya (see 'Some travellers' section below).
- Under International Health Regulations (2005), a yellow fever vaccination certificate is required from travellers over 1 year of age arriving from countries with risk of yellow fever transmission.
- According to World Health Organization (WHO), from 11 July 2016 (for all countries), the yellow fever certificate will be valid for the duration of the life of the person vaccinated. As a consequence, a valid certificate, presented by arriving travellers, cannot be rejected on the grounds that more than ten years have passed since the date vaccination became effective as stated on the certificate; and that boosters or revaccination cannot be required.
- View the WHO list of countries with risk of yellow fever transmission.
Most travellers
The vaccines in this section are recommended for most travellers visiting this country. Information on these vaccines can be found by clicking on the blue arrow. Vaccines are listed alphabetically.
Hepatitis A
Hepatitis A is a viral infection transmitted through contaminated food and water or by direct contact with an infectious person. Symptoms are often mild or absent in young children, but the disease can be more serious with advancing age. Recovery can vary from weeks to months. Following hepatitis A infection immunity is lifelong.
Prevention
All travellers should take care with personal, food and water hygiene.
Hepatitis A vaccination
As hepatitis A vaccine is well tolerated and affords long-lasting protection, it is recommended for all previously unvaccinated travellers.
Hepatitis A in brief
Tetanus
Tetanus is caused by a toxin released from Clostridium tetani bacteria and occurs worldwide. Tetanus bacteria are present in soil and manure and may be introduced through open wounds such as a puncture wound, burn or scratch.
Prevention
Travellers should thoroughly clean all wounds and seek medical attention for injuries such as animal bites/scratches, burns or wounds contaminated with soil.
Tetanus vaccination
- Travellers should have completed a tetanus vaccination course according to the UK schedule.
- If travelling to a country or area where medical facilities may be limited, a booster dose of a tetanus-containing vaccine is recommended if the last dose was more than ten years ago even if five doses of vaccine have been given previously.
Country-specific information on medical facilities may be found in the 'health' section of the FCDO foreign travel advice pages.
Tetanus in brief
Typhoid
Typhoid is a bacterial infection transmitted through contaminated food and water. Previous typhoid illness may only partially protect against re-infection.
Vaccination is recommended for most travellers, particularly travellers visiting friends and relatives, those in contact with an infected person, young children, frequent or long-stay travellers visiting areas where sanitation and food hygiene are likely to be poor, and laboratory personnel who may handle the bacteria for their work.
Prevention
All travellers should take care with personal, food and water hygiene.
Typhoid vaccination
- Oral and injectable typhoid vaccinations are available.
Typhoid in brief
Some travellers
The vaccines in this section are recommended for some travellers visiting this country. Information on when these vaccines should be considered can be found by clicking on the arrow. Vaccines are listed alphabetically.
Chikungunya
Chikungunya is a viral infection spread by mosquitoes which bite mainly during daytime hours. It causes a flu-like illness and can cause severe joint and muscles pains which usually improve in 1–2 weeks but may persist for months or years. It is rarely fatal.
Chikungunya in Kenya
There is a risk of chikungunya in this country.
Information on current outbreaks, where available, will be reported on our outbreak surveillance database.
Prevention
- Travellers should avoid mosquito bites, particularly during daytime hours.
Chikungunya vaccination
Vaccination may be considered for individuals aged 12 years of age and over who are:
- travelling to regions with a current chikungunya outbreak
- long-term or frequent travellers to regions with an increased risk of chikungunya
- exposed to the chikungunya virus through their work, such as laboratory staff working with the virus
Detailed advice about the use and contraindications of the available vaccines will be available in the green book chikungunya chapter in the coming months. For now, please see our chikungunya in brief page for details.
Chikungunya in brief
Cholera
Cholera is a bacterial infection spread by contaminated food and water. Cholera can cause severe watery diarrhoea, although mild infections are common. The risk of cholera for most travellers is low.
Prevention
All travellers should take care with personal, food and water hygiene.
Cholera vaccination
This oral vaccine is recommended for those whose activities or medical history put them at increased risk of infection or complications. This includes:
- humanitarian aid workers
- persons going to areas of cholera outbreaks who have limited access to safe water and medical care
- other travellers to cholera risk areas, for whom vaccination is considered potentially beneficial (e.g. due to their occupation, activities or underlying health problems)
Cholera in brief
Dengue
Dengue is a viral infection spread by mosquitoes which mainly feed during daytime hours. It causes a flu-like illness, which can occasionally develop into a more serious life-threatening illness. Severe dengue is rare in travellers.
The mosquitoes that spread dengue are more common in towns, cities and surrounding areas.
Dengue in Kenya
There is a risk of dengue in this country.
Information on current outbreaks, where available, will be reported on our outbreak surveillance database.
Prevention
- Travellers should avoid mosquito bites, particularly during daytime hours.
Dengue vaccination
Vaccination can be considered for individuals aged 4 years of age and older who have had dengue infection in the past and who are:
- travelling to areas where there is a risk of dengue infection or areas with an ongoing outbreak of dengue, or
- are exposed to dengue virus through their work, such as laboratory staff working with the virus
Exceptionally, vaccination can be considered in those who have not had dengue in the past. In these situations, further expert advice should be considered. Detailed guidance on how to ascertain previous infection is available in the UK Health Security Agency Immunisation against infectious disease the 'Green book'. The final decision on vaccination rests with the health professional and the traveller after a detailed risk assessment has been performed and the potential risks of vaccination explained.
Dengue in brief
Hepatitis B
Hepatitis B is a viral infection spread through blood, semen and vaginal fluids. This mostly occurs during sexual contact or as a result of blood-to-blood contact (for example from contaminated equipment during medical and dental procedures, tattooing or body piercing procedures, and sharing of intravenous needles). Mothers with the virus can also pass on the infection to their baby during childbirth.
Hepatitis B in Kenya
This country is considered to have an intermediate or high prevalence of hepatitis B.
Prevention
Travellers should avoid contact with blood or body fluids. This includes:
- Avoiding unprotected sexual intercourse.
- Avoiding tattooing, piercing, public shaving, and acupuncture (unless sterile equipment is used).
- Not sharing needles or other injection equipment.
- Following universal precautions if working in a healthcare or other higher risk setting.
A sterile medical equipment kit may be helpful when travelling to resource poor areas.
Hepatitis B vaccination
Vaccination could be considered for all travellers and is recommended for those whose activities or medical history put them at increased risk. This includes:
- Those who may have unprotected sex.
- Those who may be exposed to contaminated needles through injecting drug use.
- Those who may be exposed to blood or body fluids through their work (e.g. health and aid workers).
- Those at high risk of requiring medical or dental procedures or hospitalisation e.g. those with pre-existing medical conditions, those who may require travelling for medical care abroad, or those travelling to visit families or relatives.
- Long-stay travellers.
- Those who are participating in contact sports.
- Families adopting children from this country.
Hepatitis B in brief
Measles
Measles is a highly infectious viral illness, spread by airborne or droplet (coughing, sneezing, drops from mouth/nose) transmission. Measles usually starts with cold-like symptoms e.g. fever, cough, runny nose and conjunctivitis (sore, red eyes). This is followed by a blotchy rash starting on the face/head and spreading to the rest of the body.
Complications of measles infection can include ear infections, diarrhoea, pneumonia and convulsions (fits). Life-threatening complications such as encephalitis (brain inflammation) can occur on rare occasions. Measles can have serious consequences especially in children under 1 year of age, immunosuppressed individuals (those with a weakened immune system) and during pregnancy.
Measles in Kenya
Measles is either 'endemic' (continuous transmission in a 12-month period) and/or the measles risk is assessed to be greater than in the UK due to current outbreaks, conflict, damaged infrastructure, travel-related cases or poor vaccine coverage.
Prevention
All travellers should follow good respiratory hygiene rules and avoid contact with individuals with measles infection.
Measles vaccination
All travellers should make sure they are up to date with the measles, mumps and rubella (MMR) or measles, mumps, rubella and chickenpox (MMRV) vaccines, according to current UK recommendations.
Guidance on vaccinating adults can be found in Measles: the green book chapter – GOV.UK.
Consider early Measles Mumps Rubella (MMR)/Measles Mumps Rubella Varicella (MMRV) vaccination for infants and children.
- Infants from six months of age who are likely to be mixing with local people, should receive a MMR vaccine. The MMRV vaccine can be given from nine months of age if MMR is not available at the time of the appointment.
- Not all children will respond to MMR/MMRV given in the first year of life. When the vaccine has been given before one year of age this dose should be discounted and two further doses of MMR/MMRV should be given at the recommended ages.
- Children who are travelling and have already received one dose of MMR/MMRV at the routine age should have the second dose brought forward to at least one month after the first.
- If a child is given the second dose less than three months after the first dose and is less than 18 months of age, then the routine 18-month dose (which would constitute a third dose) should be given in order to provide optimum protection.
Measles in brief
Meningococcal disease
Invasive meningococcal disease (IMD) is a serious bacterial infection spread by close or direct contact with respiratory droplets from an infected (usually asymptomatic) person, often through coughing and sneezing or sharing cooking utensils. This is usually after lengthy and/or frequent close contact. The most common types of IMD are meningococcal meningitis (infection of the protective lining around the brain) and septicaemia (blood poisoning).
Non-invasive meningococcal disease includes conjunctivitis, which can put the individual traveller (and any of their close contacts) at risk of developing IMD.
Travellers at increased risk include health workers, people visiting friends and relatives and long-stay travellers in close contact with local people.
Meningococcal disease in Kenya
This country is part of the extended meningitis belt of sub-Saharan Africa.
Prevention
Whenever possible, travellers should avoid overcrowded conditions and follow good respiratory hygiene rules.
Meningococcal disease vaccination
Meningococcal ACWY conjugate vaccine is recommended for travellers whose activities or medical condition put them at increased risk of meningococcal disease, including:
- healthcare workers
- people visiting friends and relatives
- 'rough' travellers such as backpackers
- long-stay travellers who have close contact with local people
- travellers with certain rare immune system problems called complement disorders
- people whose spleen does not work properly (hyposplenia) or who do not have a spleen (asplenia)
Meningococcal disease in brief
Rabies
Rabies is a viral infection which is usually transmitted following contact with the saliva of an infected animal most often via a bite, scratch or lick to an open wound or mucous membrane (such as on the eye, nose or mouth). Although many different animals can transmit the virus, most cases follow a bite or scratch from an infected dog. In some parts of the world, bats are an important source of infection.
Rabies symptoms can take some time to develop, but when they do, the condition is almost always fatal.
The risk of exposure is increased by certain activities and length of stay (see below). Children are at increased risk as they are less likely to avoid contact with animals and to report a bite, scratch or lick.
Rabies in Kenya
Rabies is considered a risk and has been reported in domestic animals in this country. Bats may also carry rabies-like viruses.
Prevention
- Travellers should avoid contact with all animals. Rabies is preventable with prompt post-exposure treatment.
- Following a possible exposure, wounds should be thoroughly cleansed and an urgent local medical assessment sought, even if the wound appears trivial.
- Post-exposure treatment and advice should be in accordance with national guidelines.
Rabies vaccination
A full course of pre-exposure vaccines simplifies and shortens the course of post-exposure treatment and removes the need for rabies immunoglobulin which is in short supply world-wide.
Pre-exposure vaccinations are recommended for travellers whose activities put them at increased risk including:
- those at risk due to their work (e.g. laboratory staff working with the virus, those working with animals or health workers who may be caring for infected patients).
- those travelling to areas where access to post-exposure treatment and medical care is limited.
- those planning higher risk activities such as running or cycling.
- long-stay travellers (more than one month).
Rabies in brief
Tuberculosis
TB is a bacterial infection most commonly affecting the lungs but can affect any part of the body. When a person with TB in their lungs or throat coughs or sneezes they could pass TB on to other people. TB is curable but can be serious if not treated.
The BCG vaccination helps to protect some people, particularly babies and young children who are at increased risk from TB.
Tuberculosis in Kenya
This country has reported an annual TB incidence of greater than or equal to 40 cases per 100,000 population at least once in the last five years (further details).
Prevention
Travellers should avoid close contact with individuals known to have infectious pulmonary (lung) or laryngeal (throat) TB.
Those at risk during their work (such as healthcare workers) should take appropriate infection control and prevention precautions.
Tuberculosis (BCG) vaccination
BCG vaccine is recommended for those at increased risk of developing severe disease and/or of exposure to TB infection. See UK Health Security Agency Immunisation against infectious disease, the 'Green Book'.
For travellers, BCG vaccine is recommended for:
- Unvaccinated, children under 16 years of age, who are going to live for more than 3 months in this country. A tuberculin skin test is required prior to vaccination for all children from 6 years of age and may be recommended for some younger children.
- Unvaccinated, tuberculin skin test-negative individuals at risk due to their work such as healthcare or laboratory workers who have direct contact with TB patients or potentially infectious clinical material and vets and abattoir workers who handle animal material, which could be infected with TB.
There are specific contraindications to BCG vaccine. Health professionals must be trained and assessed as competent to administer this vaccine intradermally.
Following administration, no further vaccines should be administered in the same limb for 3 months.
The BCG vaccine is given once only, booster doses are not recommended.
Tuberculosis in brief
Yellow fever
Yellow fever is a viral infection transmitted by mosquitoes which predominantly feed between dawn and dusk, but may also bite at night, especially in the jungle environment. Symptoms may be absent or mild, but in severe cases it can cause internal bleeding, organ failure and death.
Yellow fever in Kenya
There is a risk of yellow fever transmission in parts of this country and a low potential for exposure to yellow fever in some areas (see below).
Please note: in the first half of 2022, cases of yellow fever were reported in Garissa County which is outside of the recognised yellow fever transmission area (see below for details).
Prevention
Travellers should avoid mosquito bites at all times.
Yellow fever vaccination
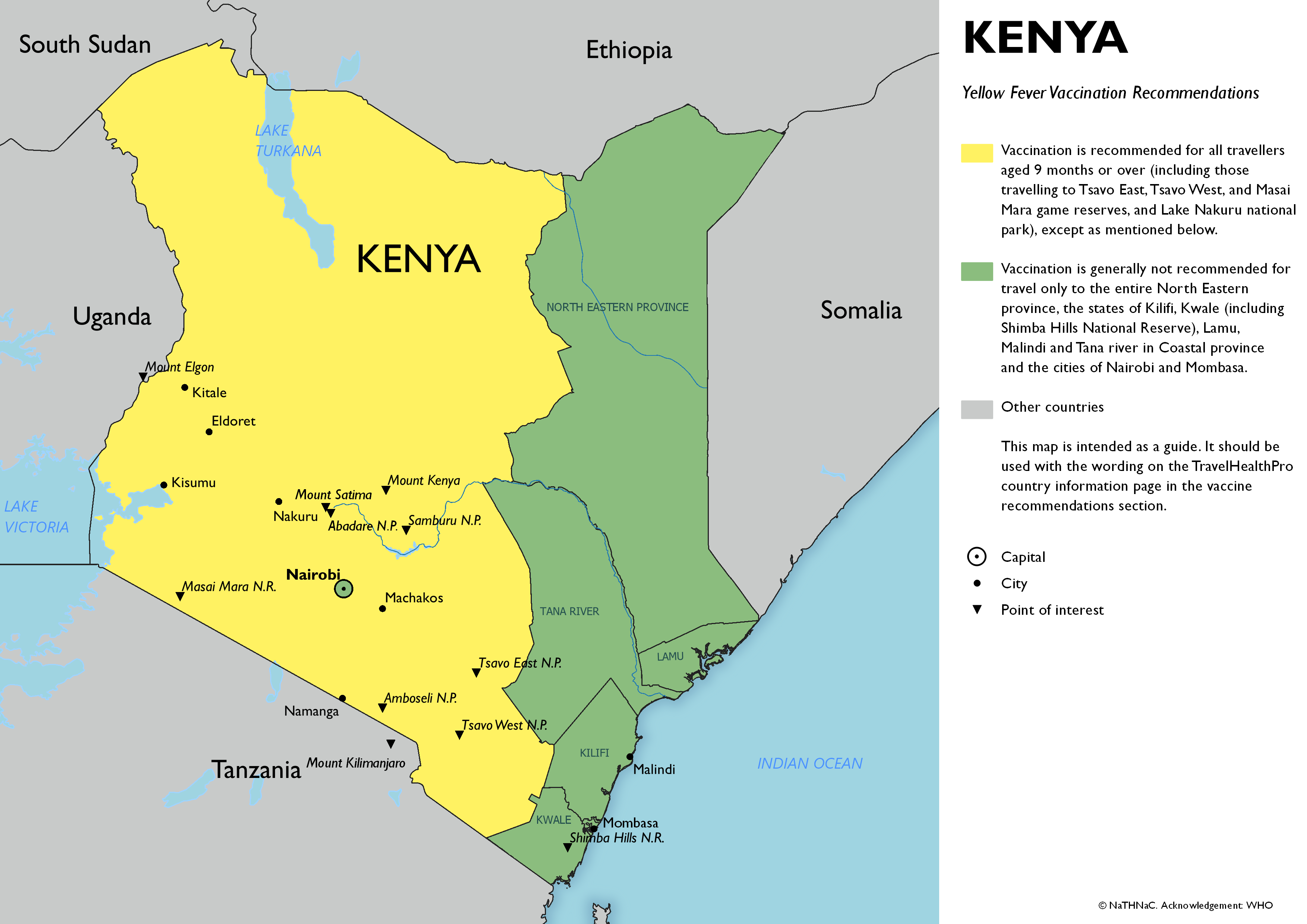
- Vaccination is recommended for travellers aged 9 months and older (including those travelling to Tsavo East, Tsavo West, and Masai Mara game reserves, and Lake Nakuru national park), except as mentioned below.
- August 2022: An outbreak of yellow fever was reported with most cases in Isiolo County. Some cases were reported in Garissa County (part of North Eastern Province) which is outside the recognised yellow fever transmission area (see map). Travellers visiting Garissa County, are encouraged to seek advice from a health professional and check the Important News and Outbreaks for updates.
Areas with low potential for exposure only (see green areas on the map):
- Vaccination is generally not recommended for travel only to areas with a low potential for exposure to yellow fever: the entire North Eastern province, the states of Kilifi, Kwale, Lamu, Malindi and Tana river in Coastal province (including Shimba Hills national park), and the cities of Nairobi and Mombasa.
- People aged 60 years or older should not be given the vaccine for travel only to areas with a low potential for exposure, due to a higher risk of life-threatening side effects.
- Vaccination could be considered for a small subset of travellers (aged 9 months to less than 60 years of age) to areas with a low potential for exposure who are at increased risk for exposure because of:
- prolonged travel.
- heavy exposure to mosquito bites.
- inability to avoid insect bites.
- See vaccine recommendation map below.
The yellow fever vaccine is not suitable for all travellers, there are specific undesirable effects associated with it. This vaccine is only available at registered yellow fever vaccination centres. Health professionals should carefully assess the risks and benefits of the vaccine, and seek specialist advice if necessary.
Yellow fever in brief
Yellow fever vaccine recommendation map for Kenya
- Click on map to open in a new window
Mpox clade I outbreak
An outbreak of mpox clade I is ongoing. Monitor the news and outbreak sections on this page for updates.
Malaria
Malaria is a serious illness caused by infection of red blood cells with a parasite called Plasmodium. The disease is transmitted by mosquitoes which predominantly feed between dusk and dawn.
Symptoms usually begin with a fever (high temperature) of 38°C (100°F) or more. Other symptoms may include feeling cold and shivery, headache, nausea, vomiting and aching muscles. Symptoms may appear between eight days and one year after the infected mosquito bite.
Prompt diagnosis and treatment is required as people with malaria can deteriorate quickly. Those at higher risk of malaria, or of severe complications from malaria, include pregnant women, infants and young children, the elderly, travellers who do not have a functioning spleen and those visiting friends and relatives.
Prevention
Travellers should follow an ABCD guide to preventing malaria:
Awareness of the risk – Risk depends on the specific location, season of travel, length of stay, activities and type of accommodation.
Bite prevention – Travellers should take mosquito bite avoidance measures.
Chemoprophylaxis – Travellers should take antimalarials (malaria prevention tablets) if appropriate for the area (see below). No antimalarials are 100% effective but taking them in combination with mosquito bite avoidance measures will give substantial protection against malaria.
Diagnosis – Travellers who develop a fever of 38°C [100°F] or higher more than one week after being in a malaria risk area, or who develop any symptoms suggestive of malaria within a year of return should seek immediate medical care. Emergency standby treatment may be considered for those going to remote areas with limited access to medical attention.
Risk areas
- There is a high risk of malaria in Kenya: atovaquone/proguanil OR doxycycline OR mefloquine recommended.
- There is very low risk in the city of Nairobi and in the highlands above 2,500m: awareness of risk and bite avoidance recommended.
Antimalarial recommendations map
- Click on map to open in a new window
Recommended antimalarials
The recommended antimalarials for Kenya are listed below. They are recommended for certain areas only (see description of risk areas above). If these are not suitable please seek further specialist advice.
Please note, the advice for children is different, the dose is based on body weight and some antimalarials are not suitable.
Atovaquone/Proguanil
Atovaquone 250mg/Proguanil 100mg combination preparation:
- start one to two days before arrival in the malaria risk area
- for adults, one tablet is taken every day, ideally at the same time of day for the duration of the time in a malaria risk area and daily for seven days after leaving the malaria risk area
- take with a fatty meal if possible
- for children paediatric tablets are available and the dose is based on body weight (see table below)
Doxycycline
Doxycycline 100mg:
- start one to two days before arrival in the malaria risk area
- adults and children over 12 years of age take 100mg daily, ideally at the same time of day for the duration of the time in a malaria risk area and daily for four weeks after leaving the malaria risk area
- take with food if possible; avoid taking this drug just before lying down
- not suitable for children under 12 years of age
Mefloquine
Mefloquine 250mg:
- this drug is taken weekly, adults take one 250mg tablet each week
- start two to three weeks before arrival in the malaria risk area and continue weekly until four weeks after leaving the malaria risk area
- for children the dose is based on the body weight (see table below)
Resources
Mpox clade I outbreak
An outbreak of mpox clade I is ongoing. Monitor the news and outbreak sections on this page for updates.
Other Risks
There are some risks that are relevant to all travellers regardless of destination. These may for example include road traffic and other accidents, diseases transmitted by insects or ticks, diseases transmitted by contaminated food and water, or health issues related to the heat or cold.
Some additional risks (which may be present in all or part of this country) are mentioned below and are presented alphabetically. Select risk to expand information.
Altitude
There is a risk of altitude illness when travelling to destinations of 2,500 metres (8,200 feet) or higher. Important risk factors are the altitude gained, rate of ascent and sleeping altitude. Rapid ascent without a period of acclimatisation puts a traveller at higher risk.
There are three syndromes; acute mountain sickness (AMS), high-altitude cerebral oedema (HACE) and high-altitude pulmonary oedema (HAPE). HACE and HAPE require immediate descent and medical treatment.
Altitude illness in Kenya
There is a point of elevation in this country higher than 2,500 metres. An example place of interest, Mt Kenya 5,199m.
Prevention
- Travellers should spend a few days at an altitude below 3,000m.
- Where possible travellers should avoid travel from altitudes less than 1,200m to altitudes greater than 3,500m in a single day.
- Ascent above 3,000m should be gradual. Travellers should avoid increasing sleeping elevation by more than 500m per day and ensure a rest day (at the same altitude) every three or four days.
- Acetazolamide can be used to assist with acclimatisation, but should not replace gradual ascent.
- Travellers who develop symptoms of AMS (headache, fatigue, loss of appetite, nausea and sleep disturbance) should avoid further ascent. In the absence of improvement or with progression of symptoms the first response should be to descend.
- Development of HACE or HAPE symptoms requires immediate descent and emergency medical treatment.
Altitude illness in brief
Biting insects or ticks
Insect or tick bites can cause irritation and infections of the skin at the site of a bite. They can also spread certain diseases.
Diseases in East Africa
There is a risk of insect or tick-borne diseases in some areas of East Africa. This includes diseases such as African Trypanosomiasis (sleeping sickness), African tick bite fever, Crimean-Congo haemorrhagic fever, leishmaniasis, Rift Valley fever and West Nile virus.
Prevention
- All travellers should avoid insect and tick bites day and night.
- There are no vaccinations (or medications) to prevent these diseases.
Further information about specific insect or tick-borne diseases for this country can be found, if appropriate on this page, in other sections of the country information pages and the insect and tick bite avoidance factsheet.
Influenza
Seasonal influenza is a viral infection of the respiratory tract and spreads easily from person to person via respiratory droplets when coughing and sneezing. Symptoms appear rapidly and include fever, muscle aches, headache, malaise (feeling unwell), cough, sore throat and a runny nose. In healthy individuals, symptoms improve without treatment within two to seven days. Severe illness is more common in those aged 65 years or over, those under 2 years of age, or those who have underlying medical conditions that increase their risk for complications of influenza.
Seasonal influenza in Kenya
Seasonal influenza occurs throughout the world. In the northern hemisphere (including the UK), most influenza occurs from as early as October through to March. In the southern hemisphere, influenza mostly occurs between April and September. In the tropics, influenza can occur throughout the year.
Prevention
All travellers should:
- Avoid close contact with symptomatic individuals
- Avoid crowded conditions where possible
- Wash their hands frequently
- Practise ‘cough hygiene’: sneezing or coughing into a tissue and promptly discarding it safely, and washing their hands
- Avoid travel if unwell with influenza-like symptoms
- A vaccine is available in certain circumstances (see below)*
*In the UK, seasonal influenza vaccine is offered routinely each year to those at higher risk of developing of severe disease following influenza infection, and certain additional groups such as healthcare workers and children as part of the UK national schedule (see information on vaccination). For those who do not fall into these groups, vaccination may be available privately.
If individuals at higher risk of severe disease following influenza infection are travelling to a country when influenza is likely to be circulating they should ensure they received a flu vaccination in the previous 12 months.
The vaccine used in the UK protects against the strains predicted to occur during the winter months of the northern hemisphere. It is not possible to obtain vaccine for the southern hemisphere in the UK, but the vaccine used during the UK influenza season should still provide important protection against strains likely to occur during the southern hemisphere influenza season, and in the tropics.
Avian influenza
Avian influenza viruses can rarely infect and cause disease in humans. Such cases are usually associated with close exposure to infected bird or animal populations. Where appropriate, information on these will be available in the outbreaks and news sections of the relevant country pages. Seasonal influenza vaccines will not provide protection against avian influenza.
Avian influenza in brief
Middle East respiratory syndrome coronavirus
MERS-CoV is a viral infection spread by direct or indirect contact with infected camels or camel-related products. Limited person to person transmission through coughing and sneezing from infected persons, typically in healthcare settings, has also been reported.
Symptoms include fever and cough that can progress to severe shortness of breath and breathing difficulties. Deaths have been reported, with the risk increasing with advancing age or underlying medical conditions.
Middle East respiratory syndrome coronavirus in Kenya
MERS-CoV has been reported to occur in camel owning households in this country.
Prevention
All travellers, particularly those with chronic medical conditions, should practise good general health measures, such as regular hand washing with soap and water at all times, but especially after visiting farms, barns or market areas. They should:
- Avoid contact with camels.
- Avoid raw camel milk and/or camel products.
- Avoid consumption of any type of raw milk, raw milk products and any food that may be contaminated with animal secretions, unless peeled and cleaned and/or thoroughly cooked.
There is currently no vaccine to prevent MERS-CoV.
MERS-CoV in brief
Outdoor air quality
Poor air quality is a significant public health problem in many parts of the world. Exposure to high levels of air pollution over short time periods (e.g. minutes/hours/days) and longer time periods (e.g. years) is linked to many different acute and chronic health problems. These effects are mainly on the respiratory (lungs and airways) and cardiovascular (heart function and blood circulation) systems.
Current information on world air quality is available from the world air quality index project.
Prevention
Travellers with health problems that might make them more vulnerable to the effects of air pollution who are travelling to areas of high pollution should:
- discuss their travel plans with their doctor, and carry adequate supplies of their regular medication.
- take sensible precautions to minimise their exposure to high levels of air pollution.
- check local air quality data and amend their activities accordingly.
- take notice of any health advisories published by the local Ministry of Health and Department for Environment, and follow the guidance provided.
It is unclear if face masks are beneficial at reducing exposure and may make breathing more difficult for those with pre-existing lung conditions. Those who choose to use one should make sure that the mask fits well and know how to wear it properly.
Outdoor air quality in brief
Schistosomiasis
Schistosomiasis is a parasitic infection. Schistosoma larvae are released from infected freshwater snails and can penetrate intact human skin following contact with contaminated freshwater. Travellers may be exposed during activities such as wading, swimming, bathing or washing clothes in freshwater streams, rivers or lakes.
Schistosomiasis infection may cause no symptoms, but early symptoms can include a rash and itchy skin ('swimmer's itch'), fever, chills, cough, or muscle aches. If not treated, it can cause serious long term health problems such as intestinal or bladder disease.
Schistosomiasis in Kenya
There is a risk of schistosomiasis in this country.
Prevention
- There is no vaccine or tablets to prevent schistosomiasis.
- All travellers should avoid wading, swimming, or bathing in fresh water. Swimming in adequately chlorinated water or sea water is not a risk for schistosomiasis.
- Drink water that is boiled, filtered or bottled.
- Application of insect repellent before exposure to fresh water, or towel drying after possible exposure to schistosomiasis are not reliable in preventing infection.
- All travellers who may have been exposed to schistosomiasis should have a health check to test for schistosomiasis infection.
Schistosomiasis in brief
Sexually transmitted infections
Sexually transmitted infections (STIs) are a group of viral, bacterial and parasitic infections spread during sexual intercourse or by intimate contact. Certain STIs can be more difficult to treat due to higher levels of antibiotic resistance and some STIs that are rare in the UK may be more common in other world regions.
Anyone who is sexually active is at risk of getting an STI wherever they are in the world.
Risk is higher for travellers who:
- have sex without a condom
- have sex with new or casual partners
- engage in sex tourism
- have sex under the influence of drugs or alcohol
Symptoms of STIs vary depending on the type of infection; some may only cause mild or unnoticeable symptoms. If symptoms do occur, they can include a rash, discharge, itching, blisters, sores or warts in genital and/or anal areas, pain when peeing and flu like symptoms.
If left untreated, STIs can cause serious long term health issues such as fertility problems, pelvic inflammatory disease and pregnancy complications.
Prevention
Using condoms consistently and correctly with new or casual partners is the most effective way to reduce risk of STIs.
Travellers can also reduce their risk of STIs by:
- ensuring they are up to date for all UK recommended vaccines, including if appropriate gonorrhoea, hepatitis B, mpox and human papillomavirus (HPV) vaccines
- considering HIV Pre-Exposure Prophylaxis (PrEP) if appropriate
Travellers should seek medical advice and give their travel history if they think they may have an STI, even if they have no symptoms. They should also have a test for STIs if they have had sex without condoms with a new or casual partner while abroad.
In the UK STI testing is free and confidential.
Zika virus
Zika virus (ZIKV) is a viral infection spread by mosquitoes which predominantly feed during daytime hours. A small number of cases of sexual transmission of ZIKV have also been reported. Most people infected with ZIKV have no symptoms. When symptoms do occur, they are usually mild and short-lived. Serious complications and deaths are not common. However, ZIKV is a cause of Congenital Zika Syndrome (microcephaly and other congenital anomalies) and neurological complications such as Guillain-Barré syndrome.
Zika virus in Kenya
There is a risk of Zika virus in this country. Details of specific affected areas within this country are not available, but information on current outbreaks where available will be reported on our outbreak surveillance database.
Pregnant women should discuss the suitability of travel and the potential risk that Zika virus may present with their health care provider.
Prevention
- All travellers should avoid mosquito bites, particularly during daytime hours.
- There is no vaccination or medication to prevent Zika virus infection.
- Women should avoid becoming pregnant while travelling in this country, and for 2 months (8 weeks) after their last possible Zika virus exposure* (see below if male partner has travelled).
- If a woman develops symptoms compatible with Zika virus infection, it is recommended she avoids becoming pregnant for a further 2 months following recovery.
- Women who visited this country while pregnant, or who become pregnant within 2 months after their last possible Zika virus exposure*, should contact their GP, obstetrician or midwife for further advice, even if they have not been unwell.
Please note screening of returning travellers without Zika virus symptoms is not available on the NHS. Couples planning pregnancy in the very near future should consider whether they should avoid travel to a country or area with risk of Zika virus, rather than delay conception for the recommended period (see below) after travel. This particularly includes couples in assisted fertility programmes.
Prevention of sexual transmission
Couples should follow guidance on prevention of sexual transmission of Zika virus and avoid conception as follows:
- If both partners travelled, for 3 months after last possible Zika virus exposure.*
- Male traveller only, for 3 months after last possible Zika virus exposure.*
- Female traveller only, for 2 months after last possible Zika virus exposure.*
See further information for pregnant women, their partners and couples planning pregnancy.
*Last possible Zika virus exposure is defined as the later of either the date of leaving a country or area with risk for Zika virus transmission, or the date on which unprotected sexual contact with a potentially infectious partner took place.
See detailed guidance on factors to consider when assessing the risk of Zika virus.
Zika virus in brief
Mpox clade I outbreak
An outbreak of mpox clade I is ongoing. Monitor the news and outbreak sections on this page for updates.
Mpox clade I outbreak
An outbreak of mpox clade I is ongoing. Monitor the news and outbreak sections on this page for updates.
Mpox clade I outbreak
An outbreak of mpox clade I is ongoing. Monitor the news and outbreak sections on this page for updates.
News
Middle East respiratory syndrome coronavirus (MERS-CoV) reminder
NaTHNaC has reviewed MERS-CoV advice for UK travellers in line with current UK Health Security Agency recommendations and is reminding travellers to be aware of their MERS-CoV risk
Changes to the Country Information pages: Zika
NaTHNaC has reviewed and updated country-specific Zika information and prevention advice
Malaria: a reminder for travellers over the winter holiday season
Advice for travellers and health professionals about malaria
Mpox clade I outbreak
An outbreak of mpox clade I is ongoing. Monitor the news and outbreak sections on this page for updates.
Outbreaks
Using information collated from a variety of sources, we regularly review and update information on overseas disease outbreaks and other health issues that may affect the UK traveller.
Please note that not all cases of disease or outbreaks are reported; some diseases may only be reported if they occur outside of the usual recognised risk area or season, or they have been reported in greater than usual numbers.
Further information on the Outbreak Surveillance section.
Mpox in Kenya
As of 23 November 2025, a total of 832 cases of mpox clade Ib (including 12 deaths), have been reported in Kenya in 2025. Please see our Topics in Brief article for further details on mpox.
Nairobi County
Migori
Cholera in Kenya
As of 17 November 2025, a total of 236 cholera cases, with six deaths, have been reported since the beginning of October 2025. Please see our Topics in Brief article for further details on cholera.
Chikungunya in Kenya
An outbreak of chikungunya has been reported in Mombasa County, June – July 2025. A total of 614 cases (97 confirmed) and no deaths were recorded. Please see our Topics in Brief article for further details on chikungunya.